Neurology & Neurosurgery - Juniper Publishers
Objectives: Recent studies reported that tumor
histopathology plays a significant role in predicting freedom from
seizures after epilepsy surgery; however, no consensus among researchers
regarding this issue exists. This study retrospectively examined
different types of tumor-related epilepsy and post-epilepsy surgical
outcomes and the relationship between various tumor Histopathology and
these outcomes.
Methods: In this hospital-based retrospective
study, patients with brain tumors and drug-resistant epilepsy, which is
defined as the failure of two tolerated and appropriately chosen
antiepileptic drugs (whether as monotherapies or in combination) to
achieve and alleviate sustained seizure freedom, were recruited. These
patients underwent a thorough pre-surgical evaluation in an Epilepsy
Monitoring Unit (EMU) before deciding to undergo surgical intervention
according to an epilepsy case management conference.
Results: One-hundred patients (including 45
children) with brain tumors were included in this study (male: female =
3:2). Most of the patients (93) had G/GNT. No significant differences in
outcome were observed among sex, age, or histopathological categories.
However, during the first year after epilepsy surgery, most of the
low-grade G/GNT cases showed favorable outcomes based on ILAE classes 1
and 2 (61.3% and 9.7%, respectively), whereas high-grade gliomas and
meningothelial tumors showed outcomes of ILAE class 1 (40% and 100%,
respectively).
Conclusion: Post-epilepsy surgical outcomes of
different brain tumors have been achieved with favorable outcomes in
children and adults with low-grade gliomas and meningiomas. Thus,
pre-surgical evaluation in EMU is highly recommended to enhance better
post-epilepsy surgical outcomes.
Keywords: Epilepsy; Brain tumor; Histopathology; Surgery; Saudi Arabia; ILAE
Approximately 30%–50% of patients with brain tumors
have epilepsy as an initial presentation [1]. However, 6%–45% of
patients with brain tumors develop seizures later in life [2,3].
Although the exact mechanism of seizure development in patients with
brain tumors is not clearly understood, recent studies have identified
that some changes in the peritumoral regions affect the release of
neurotransmitters that lead to seizure development [4]. Many studies
have reported a relationship between tumor type and seizure frequency.
For example, low-grade gliomas and glioneuronal tumors (G/GNT) are
associated with a high rate of seizure incidence (85%–92%) [5-7]. In
contrast, glioblastomas, which are high-grade tumors, are associated
with a low rate of seizure incidence (20%–50%) [8,9]. The incidence
rates of seizures in meningiomas, especially in atypical and malignant
subtypes, remain understudied [10]. Despite the abundance of knowledge
regarding surgical management of resistant forms of epilepsy, including
those associated with brain tumors, especially of the low-grade type,
prospective studies regarding the medical treatment of epilepsy in this
type of patient are scarce [11]. Reportedly, resection of the
epileptogenic zone due to the development of brain tumors lead to
freedom from or significant control of seizures in 70-90% of patients
[12,13]. Furthermore, tumor type, seizure severity, early surgical
intervention, frequency during the pre-operative stage, histopathology
of the tumors, and the extension of surgical resection to include
peritumoral tissues are reportedly the factors that increase the
likelihood of freedom from seizures post-operatively [14]. Two of the
best predictors of freedom from post-operative seizures include a
duration of less than one year since the onset of epilepsy and gross
total surgical resection [15,16]. Tumor histopathology plays a
significant role in predicting freedom from seizures after epilepsy
surgery; however, there is no consensus among researchers regarding this
issue [17,18]. This study retrospectively investigated different types
of tumor-related epilepsy and their outcomes in the first year after
epilepsy surgery.
A hospital-based retrospective study was conducted using secondary
data from the epilepsy registry at King Faisal Specialist Hospital and
Research Center (KFSH&RC) between 1998 and 2017.
The included patients underwent surgery for
drug-resistant epilepsy. The patients were admitted to the Epilepsy
Monitoring Unit (EMU) for long-term monitoring; they underwent
presurgical evaluations such as surface electroencephalography (EEG),
3-tesla magnetic resonance imaging (MRI) of the brain, and
fluoro-deoxy-glucose positron emission tomography (PET) brain scans.
Additionally, a qualified neuropsychologist was present during the
evaluation of the enrolled patients with epilepsy. In some patients,
intracranial subdural recordings, intracarotid amobarbital procedure
(Wada test) and electrocorticography (ECoG), and motor, sensory, and
language mapping were performed.
Detailed information about the patients was
collected. This information included demographic characteristics (age,
gender, handedness, age at onset of the disease) and history and
clinical data (type of seizure and frequency, seizure observed at EMU,
MRI findings, PET scan, ictal EEG (IEEG) location and type, subdural EEG
recording, and inter-ictal EEG [IIEEG] location and type). Moreover,
final diagnosis, surgical procedures, and pathology were recorded as the
primary outcome. All tumor cases enrolled in this study were reviewed
and graded independently by a neuropathologist according to the World
Health Organization (WHO) classification [19]. Epilepsy data were
discussed in an epilepsy surgery conference with epileptologists,
epilepsy surgeons, neuroradiologists, and neuropsychologists to
determine the status and surgical candidacy of the patient.
According to the International League Against
Epilepsy (ILAE) commission report (1997–2001), six outcomes of interest
were proposed [20]. However, the categories 4, 5, and 6 are difficult to
measure and implement in daily practice, particularly when parameters
related to the quality of life are included. Hence, we suggested
simplifying the ILAE classification of epilepsy surgical outcomes with
only four categories rather than six to facilitate its application for a
new modification that shares the ILAE classification for classes 1, 2,
and 3, while classes 4, 5, and 6 would be merged into only one class,
called class 4. Thus, the definitions of the classes were divided into
four groups:
1. class 1, patients who were completely seizure-free with no auras;
2. class 2, patients with auras but no seizures;
3. class 3, patients experiencing one to three seizure days per year ±auras; and
4. class 4, ranging from four or more seizure days
per year to those experiencing ≥ 50% reduction of baseline seizure days
±auras to ≥ 100% increase in baseline seizure days; ±auras. Furthermore,
outcomes of classes 1 and 2 were considered favorable, while those of
classes 3 and 4 were considered unfavorable. These four outcomes were
investigated during the first post-surgical year.
Statistical analysis through cross-tabulation of the tumor groups,
pathologies, and progressive outcomes was performed using SAS software
(ver. 9.4). Due to the small sample size, some subgroups, pathologies,
and outcomes were collapsed. Proportional statistics, and chi-square and
Fisher’s exact test were used to explain the findings within a 95%
confidence interval (CI). A P-value of < 0.05 was considered
statistically significant.
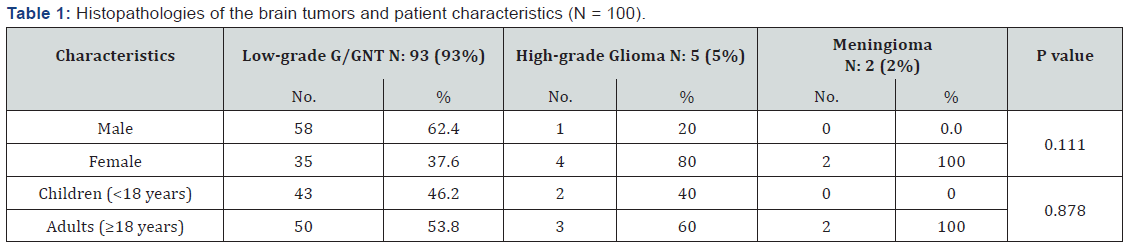
Among the 100 patients with brain tumors related
epilepsy included in this study, 59 (59%) were males, and 41 (41%) were
females. The incidence of brain tumor-related epilepsy (BTRE) in our
center was lower among children than adults (45% versus 55%). However,
the differences among sex, age, and the histopathology categories were
not statistically significant (P = 0.111 and 0.878, respectively) as
depicted in Table 1.
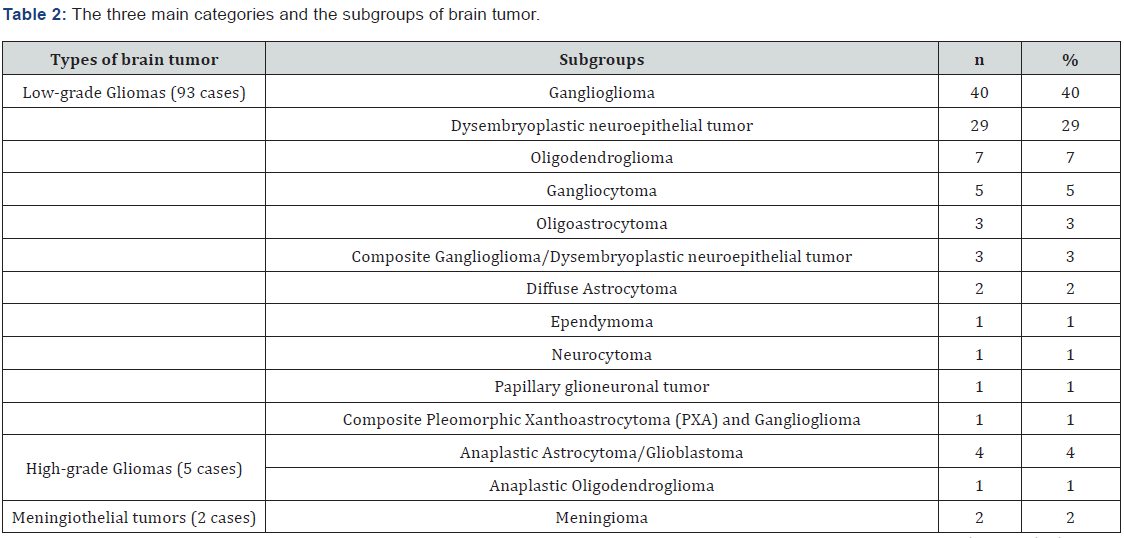
According to histopathological findings, the cases of
brain tumors were grouped into three main categories (Table 2). Most of
the tumors (93%) were low-grade gliomas or glioneuronal tumors (G/GNT)
followed by high-grade gliomas (5%); only two meningioma cases (2%) were
detected. Among the three main categories of brain tumors, low-grade
G/GNT consisted of 11 entities. Under this category, 40 tumors were
gangliogliomas, and 29 tumors were Dysembryoplastic neuroepithelial
tumors (DNET). Among the five high-grade gliomas, three were astrocytic
tumors. Interestingly, only two meningiomas were found. Table 2 details
the pathological categories.
In this study, the primary postoperative outcome was
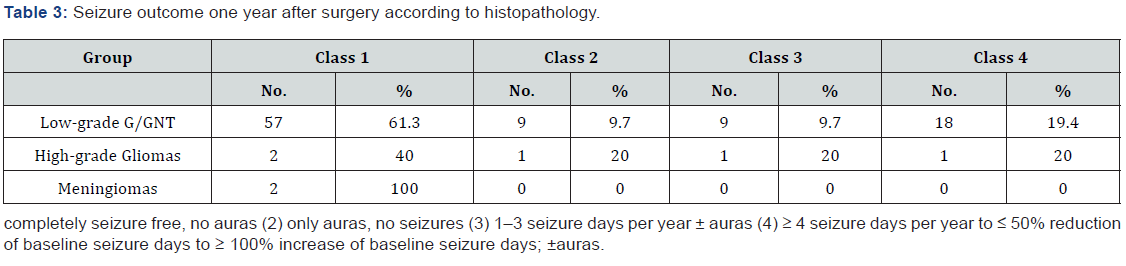
evaluated using the modified ILAE classification described in the
methodology section. During the first post-surgical year, most patients
with low-grade G/GNT experienced favorable outcomes (classes 1 and 2,
61.3% and 9.7%, respectively) as shown in Table 3. In contrast,
approximately 40% of the patients with high-grade gliomas showed
favorable outcomes (ILAE class 1). Both meningioma cases (100%) showed
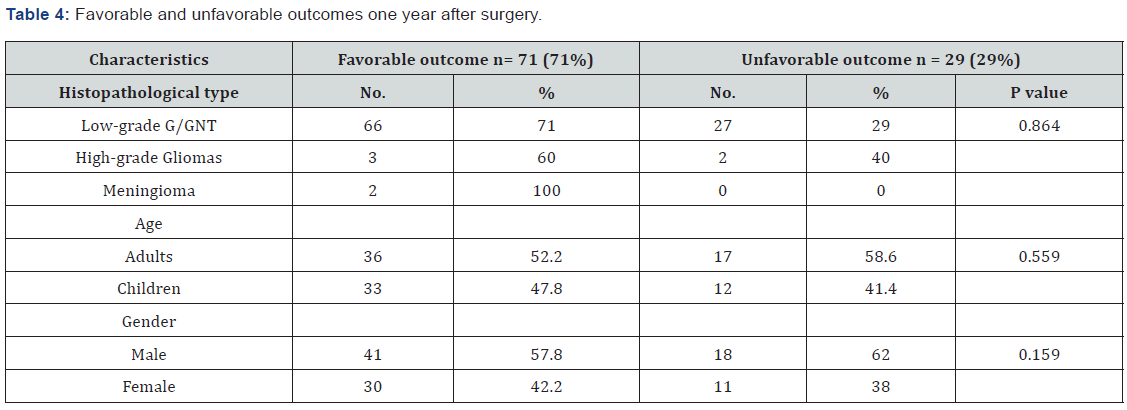
outcomes of ILAE class 1. Among the 100 patients with brain tumors, 71
(71%) patients, including 66 patients with low-grade G/GNT, three
patients with high-grade gliomas, and two patients with meningiomas,
experienced favorable outcomes during the one-year post-surgical period
(Table 4). Moreover, the incidence of favorable outcome was higher in
adult patients than in children (52.2% versus 47.8%) and in male versus
female patients (41% versus 30%). However, these differences in outcome
dependent on histopathological type, age, and sex were not statistically
significant (P = 0.864, 0.559, and 0.159, respectively).
From the epilepsy registry at KFSH&RC, 100
patients who underwent surgery for tumor-related epilepsy were included
in this study. Varying associations between different brain tumor types
and epilepsy have been reported. Most studies show gangliogliomas to be
the most common tumor type associated with epilepsy, followed by DNET,
oligodendrogliomas, and astrocytomas [21-24]. These findings support our
results, that is, most of our patients had low-grade G/GNT (93.0%),
most of which were gangliogliomas (40%) followed by DNET (29%).
Furthermore, Babini et al. reported that gangliogliomas (66.7% versus
40%) [25] were the most frequent tumors among their patients; however,
their sample size was smaller (30 cases) than in our study. Contrary to
our findings, Kahlenberg et al. reported that mixed oligo-astrocytomas
were the most prevalent tumors followed by astrocytomas grade II and
oligodendrogliomas of grade II [25]. The incidence of high-grade gliomas
was lower (5%) in our study than in a study by Michelucci et al. in
Italy (77.0%), a finding attributed to a significantly high prevalence
of high-grade gliomas in that area [15].
Seizures have a great impact on patient and caregiver
quality of life. Seizures affect all aspects of a patient’s life, such
as employment, social life, driving, and entertainment. Epilepsy surgery
as described in many recent studies, is considered to relieve
tumor-related epilepsy and achieve favorable outcomes [15,26,27].
However, in some cases, epilepsy persist even after resecting the
primary focus [25]. All of our patients underwent well-planned epilepsy
surgery, which is defined as the resection of the tumor and peritumoral
tissues [23]. Consequently, our patients showed varying degrees of
improvement during the first post-surgical year depending on the type of
brain tumor (low-grade G/GNT versus high-grade gliomas); however, the
differences were not statistically significant (P = 0.864). For example,
patients with low-grade tumors, which were the most common type of
tumor in our study (93 cases), showed a favorable outcome during the
first post-epilepsy surgery year with approximately 71% freedom from
seizure (classes 1 and 2). Michelucci et al. reported findings that were
similar to our study, that is, better outcomes was observed in patients
with low-grade gliomas (76%) [15]. In contrast, Kahlenberg et al.
showed that about half of their patients (30 out of 54; 55.6%) with
brain tumor-related epilepsy showed good post-surgical outcomes
(seizure-free periods > 12 months) [25]. These proportions were lower
than those observed in our study (55.6% versus 71%).
In our opinion, the ILAE classification of epilepsy
surgical outcomes should be simplified using only four categories rather
than six to facilitate ILAE application. Hence, whenever patients have
four or more seizures (outcomes 4, 5, and 6), they should be classified
into one category (category 4). The currently used ILAE Commission on
Neurosurgery in 2001[28] still has some elements that make the use of
categories 4, 5, and 6 difficult to measure and implement in daily
practice, particularly when including parameters related to quality of
life. This new modified classification can help the researchers in their
ongoing studies.
Furthermore, few patients in our study had high-grade
gliomas (five) or meningiomas (two). These patients showed a favorable
outcome during the first post-surgical year (60% and 100%,
respectively). Michelucci et al. reported similar results in which 58%
of their patients with high-grade glioma became seizure free after tumor
removal [15].
Pediatric and adult groups showed no significant
differences regarding seizure outcomes during the first post-surgical
year (P = 0.559); thus, we cannot claim that surgery is more beneficial
in pediatric patients. These findings were similar to those of other
studies [23].
Our study has three main limitations:
1. the sample size was small and included only five
patients with high-grade gliomas and two patients with meningothelial
tumors (two cases); this made comparison with low-grade G/GNT
insufficient although our sample size (100 cases) is comparable to that
of other studies;
2. this series of tumor-related epilepsy does not
represent the population with epilepsy in Saudi Arabia because not all
patients with tumor-related epilepsy are eligible to be admitted to our
institution, and thus, they are treated; and
3. the possibility of bias occurring during data
collection in a retrospective study. Despite the above-mentioned
limitations, we hope that our study provides valuable information on one
of the most debatable topics in epilepsy surgery in the country and
throughout the Middle East.
In this study, the most common tumor-related epilepsy
was low-grade G/GNT. Outcomes of post epilepsy surgery of different
brain tumors have been achieved with a favorable outcome in both
children and adults. Thus, thorough pre-surgical evaluation of patients
with brain tumor-related epilepsy in EMU is highly recommended to
enhance better post-epilepsy surgical outcomes. Further prospective,
multicenter studies are needed with a larger number of patients to allow
the findings to be more generalizable in Saudi Arabia.
Click here: https://juniperpublishers.com/index.php